Nebraska Recommendations: Conducting Faith-Based Services
-
Sierra Salgado Pirigyi
- Published on
Faith leaders need to communicate clearly to their communities what it will take in order to reopen. It is entirely reasonable, especially for very large communities, to say that they are unable to restart just yet because of extensive community transmission. With different communities doing different things, the situation is ripe for this to be a source of conflict or confusion. So, communication is absolutely key. It will be important to communicate what it will take to reopen your parishes:
The Omaha Interfaith Community offers the following general considerations to help communities of faith discern how best to practice their beliefs while keeping their staff and congregations safe. Millions of Americans embrace worship as an essential part of life. For many faith traditions, gathering together for worship is at the heart of what it means to be a community. But as Americans are now aware, gatherings present an increased risk for spread of COVID-19 during this Public Health Emergency and many congregants and staff may be at higher risk of severe disease if they become infected.
The Omaha Interfaith Community offers these suggestions based on review of numerous documents for faith communities to consider and accept, reject, or modify, consistent with their own faith traditions, in the course of preparing to reconvene for in-person gatherings while still working to prevent the spread of COVID-19. We also note that a church in Omaha chose to close on June 5th, when a staff member was tested positive despite following state, county, and city guidelines to reopen. There are additional examples of outbreaks in churches in states that have reopened.
PRIME DIRECTIVES
- Designate a staff person to be responsible for responding to COVID-19 concerns. Staff, clergy, volunteers, and congregants should know who this person is and how to contact them if they become sick or are around others diagnosed with COVID-19. This person should also be aware of state or local regulatory agency policies related to group gatherings.
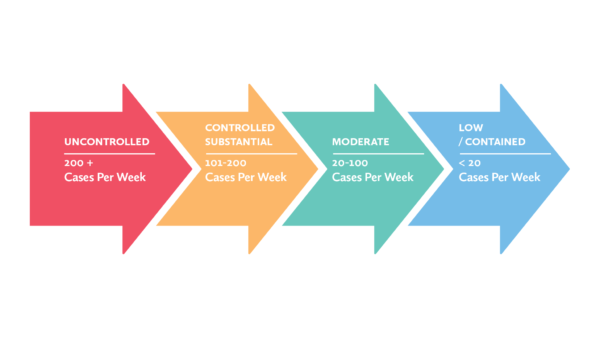
- Understand current levels of community transmission. Is it controlled or uncontrolled. If controlled, is there substantial, moderate or low transmission in your community.
- Faith communities are encouraged to continue the use of video and other streaming technologies to allow members of their communities to remain connected to the larger community without being physically present until their elected officials contain the spread of COVID in their communities as being done successfully in Asia, Oceania, and Europe.
- Establish and maintain communication with local and State authorities to determine current levels of community mitigation. They may frame this as phases of reopening. Please note that these reopening guidelines are often politically determined and may be independent of actual disease risk in the community.
- Review local and state guidelines for faith-based organizations.
- Review your facility plans including the size of the building, all points of entry, and air handling systems to understand how to implement social distancing and maximize air flow.
- Assess the health status of your staff and congregants as voluntarily shared or based on basic demographics as the age distribution.
- Provide protections for staff and congregants at higher risk for severe illness from COVID-19. Offer options for staff at higher risk for severe illness (including older adults and people of all ages with certain underlying medical conditions) that limit their exposure risk. Offer options for congregants at higher risk of severe illness that limit their exposure risk (e.g., remote participation in services).
- Encourage any organizations that share or use the facilities to also follow these considerations as applicable.
LOGISTICAL BENCHMARKS
- We encourage that congregant services begin no sooner than there is controlled moderate community transmission of <26 cases/million population/day in their community. For Omaha, Douglas county (pop. 570,000), that would represent fewer than 14 cases a day . The number of cases can be checked on the Omaha COVID tracker. The size of gathering can then be adjusted based on local/state guidelines and actual community transmission. Note again that size limitations will also be affected by your physical space to permit social distancing.
- We encourage that vulnerable populations refrain from attending services in-person until there is only low level community transmission of less than 5 cases/million population/day with adequate testing measures and sufficient community healthcare and public health surge
capacity to deal with an increase in cases. That would be less than 3 COVID-19 cases in Douglas county a day. - We recommend no singing or use of wind instruments without additional precautions until there is only low level community transmission (less than 5 cases/day in Douglas county per day).
PRACTICAL CONSIDERATIONS
Assess the following as key markers that communities need to hit in order to be comfortable in managing this new situation that will likely be our new normal for some months:
- How many volunteers under a certain age?
- How many ushers or security personnel?
- What supplies will be needed, and how many people on cleaning crews?
- What kinds of change in service schedules will be needed, or dividing the congregation throughout the week?
SAFETY ACTIONS
Promote healthy practices to limit disease transmission.
- Actively discourage ill persons to attend. Encourage staff or congregants who are sick or who have had close contact with a person with COVID-19 to stay home. Share CDC’s criteria for staying home with staff and congregants so that they know how to care for themselves and others. Consider posting signs at entrances with this information.
- Encourage use of cloth face coverings among staff and congregants. Note: Cloth face coverings should not be placed on children younger than 2 years old, anyone who has trouble breathing or is unconscious, and anyone who is incapacitated or otherwise unable to remove the cloth face covering without assistance. Cloth face coverings are meant to protect other people in case the wearer is unknowingly infected but does not have symptoms. Ideally they are multilayered.
- Promote social distancing.
- Encourage staff and congregants to maintain good hand hygiene, washing hands with soap and water for at least 20 seconds.
- Have adequate supplies to support healthy behaviors, including masks, soap, hand sanitizer with at least 60 percent alcohol (for those who can safely use hand sanitizer), tissues, and no-touch trash cans.
- Encourage staff and congregants to cover coughs and sneezes with a tissue or use the inside of their elbow. Used tissues should be thrown in the trash and hands washed.
- Whenever soap and water are not readily available, hand sanitizer with at least 60% alcohol can be used.
- Consider posting signs on how to stop the spread of COVID-19 and how to promote everyday protective measures, such as properly wearing a face covering, washing hands, and covering coughs and sneezes.
PROMOTE WEARING FACE MASKs
- Encourage use of cloth face coverings among staff and congregants. Note: Cloth face coverings should not be placed on children younger than 2 years old, anyone who has trouble breathing or is unconscious, and anyone who is incapacitated or otherwise unable to remove the cloth face covering without assistance. Cloth face coverings are meant to protect other people in case the wearer is unknowingly infected but does not have symptoms. Ideally they are multilayered.
PROMOTE SOCIAL DISTANCING
- Take steps to limit the size of gatherings in accordance with the guidance and directives of state and local authorities and subject to the protections of the First Amendment and any other applicable federal law.
- Promote social distancing at services and other gatherings, ensuring that clergy, staff, choir, volunteers and attendees at the services follow social distancing, as circumstances and faith traditions allow, to lessen their risk.
- Seating in houses of worship should be arranged in such a way as to maintain appropriate social distancing between parties. A “party” should be understood to include members of a household who live together and therefore may be seated together in the house of worship, but should maintain six feet of social distance from other parties.
- It is essential for the safety of those attending services that their arrival and departure be managed in such a way as to prevent interaction between parties. Appropriate steps should be taken to dismiss and pace the departure of those present at the conclusion of the service so as to prevent the interaction between parties as distances less than six feet.
- Faith communities are encouraged to add additional service times to allow for appropriate social distancing. Where appropriate, the use of overflow rooms and the continuation of drive- in services can be effective in maintaining proper social distancing.
- Consider holding services and gatherings in a large, well-ventilated area or outdoors, as circumstances and faith traditions allow.
Consider appropriate mitigation measures, including taking steps to limit the size of gatherings maintaining social distancing, at other gatherings such as funerals, weddings, religious education classes, youth events, support groups and any other programming, where consistent with the faith tradition. - Provide physical guides, such as tape on floors or walkways and signs on walls, to ensure that staff and children remain at least 6 feet apart in lines and at other times (e.g. guides for creating “one-way routes” in hallways).
- Consider establishing a reservation system (e.g book a table) for attending services to ensure social distancing and maintaining the list of congregants and staff for 2 weeks to facilitate any subsequently required contact tracing.
INTENSIFY CLEANING, DISINFECTION, AND VENTILATION
- Clean and disinfect frequently touched surfaces at least daily and shared objects in between uses. Standard guidelines for Cleaning and Disinfection including EPA-registered disinfectants can be found here.
- Develop a schedule of increased, routine cleaning and disinfection.
- Avoid use of items that are not easily cleaned, sanitized, or disinfected.
- Ensure safe and correct application of disinfectants and keep them away from children.
- Cleaning products should not be used near children, and staff should ensure that there is adequate ventilation when using these products to prevent children or themselves from inhaling toxic fumes.
- Ensure that ventilation systems operate properly and increase circulation of outdoor air as much as possible by opening windows and doors, using fans, etc. Do not open windows and doors if they pose a safety risk to children using the facility.
- The use of staff or volunteers to hold open doors to the house of worship so that those attending are not touching common door handles is highly encouraged.
- If your faith community offers multiple services, consider scheduling services far enough apart to allow time for cleaning and disinfecting high-touch surfaces between services in addition to common areas and restrooms. Take steps to ensure that all water systems and features (for example, drinking fountains, decorative fountains) are safe to use after a prolonged facility shutdown to minimize the risk of Legionnaires’ disease and other diseases associated with water.
Take steps to minimize community sharing of worship materials and other items
- Consistent with the community’s faith tradition, consider temporarily limiting the sharing of frequently touched objects, such as worship aids, prayer rugs, prayer books, hymnals,
religious texts and other bulletins, books, or other items passed or shared among congregants, and encouraging congregants to bring their own such items, if possible, or photocopying or projecting prayers, songs, and texts using electronic means. - Modify the methods used to receive financial contributions. Consider a stationary collection box, or electronic methods of collection instead of shared collection trays or baskets.
- If food is offered at any event, consider pre-packaged options, and avoid buffet or family-style meals if possible.
Religious services that include a distribution of communion are highly encouraged to adhere to additional precautions including:
- Faith traditions that allow for the use of pre-packaged communion elements are encouraged to do so.
- The use of a common communion cup shared between parties is not permitted.
- Sound medical judgement would require that any person involved in the distribution of communion first thoroughly wash and sanitize his/her hands.
- Prudent implementation of social distancing would highly suggest that persons receiving communion from a faith leader should do so in single file lines (not side by side) with six feet of distancing between persons. Releasing one row at a time for communion will prevent long lines from forming that would compromise social distancing.
NURSERY / CHILDCARE
- If a nursery or childcare will be provided during services and events, refer to CDC’s information on preventing the spread of COVID-19 in childcare settings and adapt as needed for your setting.
- If holding summer day camps, refer to CDC’s information on youth and summer camps and adapt as needed.
STAFFING AND TRAINING
- Train all clergy and staff in the above safety actions. Consider conducting the training virtually, or, if in-person, ensure that social distancing is maintained.
MONITORING AND PREPARING
- Plan for when a staff member or congregant becomes sick.
- Identify an area to separate anyone who exhibits symptoms of COVID-19 during hours of operation, and ensure that children are not left without adult supervision.
- Establish procedures for safely transporting anyone who becomes sick at the facility to their home or a healthcare facility.
- Notify local health officials if a person diagnosed with COVID-19 has been in the facility and communicate with staff and congregants about potential exposure while maintaining confidentiality as required by the Americans with Disabilities Act (ADA) or other applicable laws and in accordance with religious practices.
- Advise those with exposure to a person diagnosed with COVID-19 to stay home and self-monitor for symptoms, and follow CDC guidance if symptoms develop.
- Close off areas used by the sick person and do not use the area until after cleaning and disinfection. Ensure safe and correct application of disinfectants and keep disinfectant products away from children.
- Advise staff and congregants with symptoms of COVID-19 or who have tested positive for COVID-19 not to return to the facility until they have met CDC’s criteria to discontinue home isolation.
MAINTAIN HEALTHY OPERATIONS
- Implement flexible sick leave and related flexible policies and practices for staff (e.g., allow work from home, if feasible), and provide requested reasonable accommodation absent undue hardship to individuals with disabilities under the Americans with Disabilities Act (ADA) or other applicable laws and in accordance with religious practices.
- Monitor absenteeism and create a roster of trained back-up staff.
- As volunteers often perform important duties (e.g., greeters, ushers, childcare), consider similar monitoring, planning, and training for them. Consider that volunteer and staffing may need to increase to implement cleaning and safety protocols and to accommodate additional services with reduced attendance.
- Communicate clearly with staff and congregants about actions being taken to protect their health.
SIGNS AND MESSAGES
- Post signs in community-appropriate languages in highly visible locations (e.g., entrances, restrooms, gathering halls/community rooms/gyms) that promote everyday protective measures and describe how to stop the spread of germs (such as by properly washing hands and properly wearing a cloth face covering).
- Include opportunities for verbal messaging, descriptions, or tours for persons with low levels of literacy.
- Include messages (for example, videos) about behaviors that prevent the spread of COVID-19 when communicating with staff and congregants (such as in emails and on community websites and social media accounts).
Find freely available CDC print and digital resources on CDC’s communications resources main page.
Spread the Word
